
Improving Quality Through Courageous, Coaching Conversations
13th January 2026
Improving Quality Through Courageous, Coaching Conversations
Sarah Nerva, Operational Team Lead at Newham Community Integrated Mental Health Service (North) & a QI Coach reflects on her experience of leading her team through a challenging period of transition, and shares what she has learnt about the soft skills that are needed to set a team up for successful improvement work.
Creating a culture for improvement
CIMHS North was the focus of significant improvement work in 2023-24. Progress was initially hindered by organisational cultural differences and systemic issues, but the team went on to successfully implement a co-designed recovery plan focused on clinical efficiency, staff wellbeing, and operational safety and have been shortlisted for an HSJ Award.
When we think about Quality Improvement, the first things to spring to mind may be tools such as Driver Diagrams and Plan Do Study Act Cycles, or the use of data over time. But, improving quality isn’t just a technical pursuit; it’s a human one. While tools and data are fundamental to QI, the real engine of transformation lies in how people communicate, collaborate, and lead.
The first step in CIMHS’ improvement journey was creating a culture in which the team felt supported and empowered to change how they delivered their services. The courage to have difficult conversations, the creation of psychological safety, and the adoption of a coaching mindset are the essential foundations of a culture where quality can thrive.
The Role of Difficult Conversations in Healthcare Quality
Healthcare professionals often navigate sensitive conversations with patients and carers. Yet, when it comes to interpersonal dynamics within healthcare teams, such as addressing underperformance, work ethic, or concerns about the quality of care being provided, many avoid the discomfort of difficult conversations. The result? The acceptance of mediocre practice, and avoidance where accountability is needed.
Whether it’s a nurse hesitant to challenge doctor’s decision, or a manager reluctant to address burnout in their team, the cost of avoidance is steep. Delayed interventions and compromised patient care can all stem from people shying away from difficult discussions. Improvement can’t take place unless there is acknowledgement of a problem in the first place. So, when leaders and clinicians lean into these conversations with compassion and practice radical candour – giving honest, direct feedback with kindness and empathy, they unlock the potential for real-time learning, stronger relationships, and safer systems.
Starting a difficult conversation can be nerve-wracking, so here are some tips for creating space for meaningful conversations at work:
- Leave the Agenda at the Door
Rather than arriving with a rigid checklist of topics to cover, approach the conversation with curiosity and openness. Let the dialogue unfold organically. You might discover that the other person is navigating challenges that are impacting their wellbeing. Take a moment at the start to check in; simply asking “How are you doing?” can open the door to deeper, more meaningful exchange. - You’re Not Expected to Solve Everything Right Away
Initiating the conversation is often the hardest, and most important, step. You don’t need to have all the answers immediately. What matters is creating a space where ongoing dialogue can happen. Solutions can emerge over time. - It’s a Learning Process for Everyone
There’s no perfect script or policy for navigating these kinds of discussions. Both parties are learning, adapting, and growing. Conversations are a chance to build mutual understanding, not to perform or have it all figured out. - Don’t Overlook the Small Stuff
Difficult conversations aren’t always about major issues. Sometimes, it’s the smaller, day-to-day discomforts that need addressing. Addressing these “small” topics with honesty and care can prevent them from becoming larger problems down the line. - Prioritise Psychological Safety
For any conversation to be truly effective, both people need to feel safe to speak honestly, ask questions, admit uncertainty, and express emotions without fear of judgment or consequence. Psychological safety is the foundation of all meaningful dialogue and is essential in building trust and connection over time.
Psychological Safety: The Bedrock of Honest Dialogue
Psychological safety, defined by Harvard professor Amy Edmondson as “a belief that one will not be punished or humiliated for speaking up with ideas, questions, concerns, or mistakes” is a prerequisite for quality improvement. In environments where staff fear blame, errors go unreported, people are scared to test new ways of working, and morale suffers.
Creating psychological safety in healthcare means more than encouraging feedback. It requires modelling vulnerability, actively listening, and responding with curiosity rather than judgment. When a non-registered professional such as a Community Connector feels safe to question a protocol, or a new member of a team feels empowered to suggest a workflow improvement, the entire system benefits.
Signs of a psychologically unsafe environment include:
- Reluctance to speak up in meetings
- Blame-heavy incident reviews
- Hierarchical communication that discourages dissent
Shifting this culture starts with leadership. Leaders must consistently demonstrate that speaking up is valued, not penalised; and that learning, not perfection, is the goal.
The Coaching Approach: Empowerment Over Instruction
Traditional management in healthcare is often hierarchical and directive: telling people what to do and how to do it. A coaching mindset invites reflection, rather than giving answers. It’s about asking powerful questions, listening deeply, and helping individuals uncover their own insights. This approach fosters ownership, accountability, agency, resilience, and continuous learning. All key ingredients for sustainable quality improvement.
Examples of coaching in action:
- A team manager asking, “What do you think is contributing to the increased waiting list?” rather than prescribing a solution
- A supervisor helping a newly qualified nurse reflect on a challenging patient interaction through open-ended questions
- A team debrief that focuses on what went well and what could be improved, rather than who was at fault
Conclusion: Culture as the Ultimate Quality System
Quality Improvement in healthcare is often framed as a technical challenge. But the truth is, it’s a cultural one. By embracing difficult conversations, fostering psychological safety, and leading with compassion and a coaching mindset, healthcare organisations can build environments where excellence isn’t just expected, it’s inevitable.
Over the past two years in CIMHS North, key changes have included a re-design of the referral process, the introduction of daily safety huddles, and distributed leadership. These efforts have helped the team to see 85% of patients within 28-days of referral, halve treatment waiting times, reduce agency costs by £666,000 annually, and improve staff and service user experience. Collaborative work with community partners, service users, and public health have helped drive sustainable improvement, highlighting a model of integrated, inclusive mental health care transformation. The team are delighted to be nominated for an HSJ Award under the ‘Performance Recovery Award’ category.
The impact of a culture on outcomes: I-Charts showing the improvement in waiting times for assessment and treatment in CIMHS North.
So, the next time you feel the urge to avoid a tough conversation, pause. That discomfort might just be the first step to better care, stronger teams, and a safer system.
Most Read Stories
-
Why is Quality Control important?
18th July 2018

-
2016 QI Conference Poster Presentations
22nd March 2016
-
Recognising Racism: Using QI to Help Take Action
21st January 2021

-
QI Essentials: What does a Chief Quality Officer do?
18th March 2019

-
Using data enabled us to understand our problem
31st March 2023

-
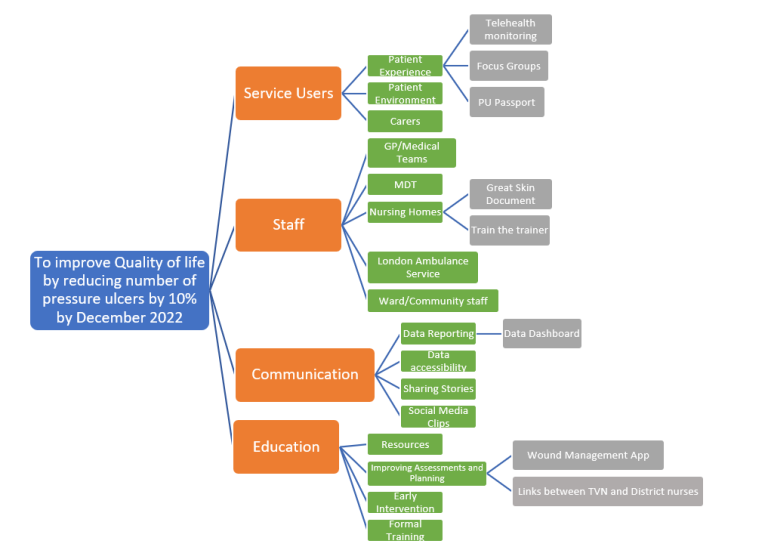
The Power of Data in Reducing Pressure Ulcers
12th January 2022

Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.



