Making It Easier to Attend: Improving Access in the Tower Hamlets Continence Service
8th April 2026
Written by Gifty Achaempong (Continence Nurse Specialist), Rosemary Ndungu (Continence Nurse Specialist), Nkechi Ochulo (Continence Nurse Specialist) and Chloe Preston (Improvement Advisor)

Missed appointments are a familiar challenge across the NHS, but behind every “Did Not Attend” is a story.
For the Tower Hamlets Continence Service, missed appointments weren’t just numbers on a chart. They represented missed opportunities for care, delays in treatment, and frustration for both service users and staff. In a service supporting people with continence needs, often a sensitive and under-discussed area of health, every missed appointment risked leaving someone without the support they needed to maintain dignity, independence, and quality of life.
Starting with what the data told us
In early 2025, the team noticed that the percentage of missed face to face appointments throughout 2024 were consistently high, averaging nearly 27%. This meant that more than 1 in 4 service users were not attending their appointments. The team also recognised that missed appointments peaked around certain times of the year, including Ramadan and school holidays.
This pattern prompted an important question in the team: What is really driving missed appointments in our service?
The team recognised that while data can highlight the problem, it is people’s experiences that help explain it.
Listening to what matters to service users
To move beyond assumptions, the team heard directly from service users. The findings revealed a mix of practical barriers and personal circumstances.
Some people spoke about simply forgetting appointments or feeling that they were no longer needed. Others described not receiving letters or text reminders, or finding it difficult to cancel or rearrange when circumstances changed. Long gaps between booking and appointment made it harder for people to stay engaged or even remember they had been referred.
For many, the barriers were more practical and deeply rooted in daily life. Work commitments, transport challenges, and the absence of carers or family support made attending difficult. Clinic times often did not align with people’s routines, and for some, the effort required to attend outweighed the perceived benefit.
These insights made one thing clear: missed appointments were not simply a matter of choice, they were often the result of systems that did not fully work for the people using them.
Testing what could make a difference
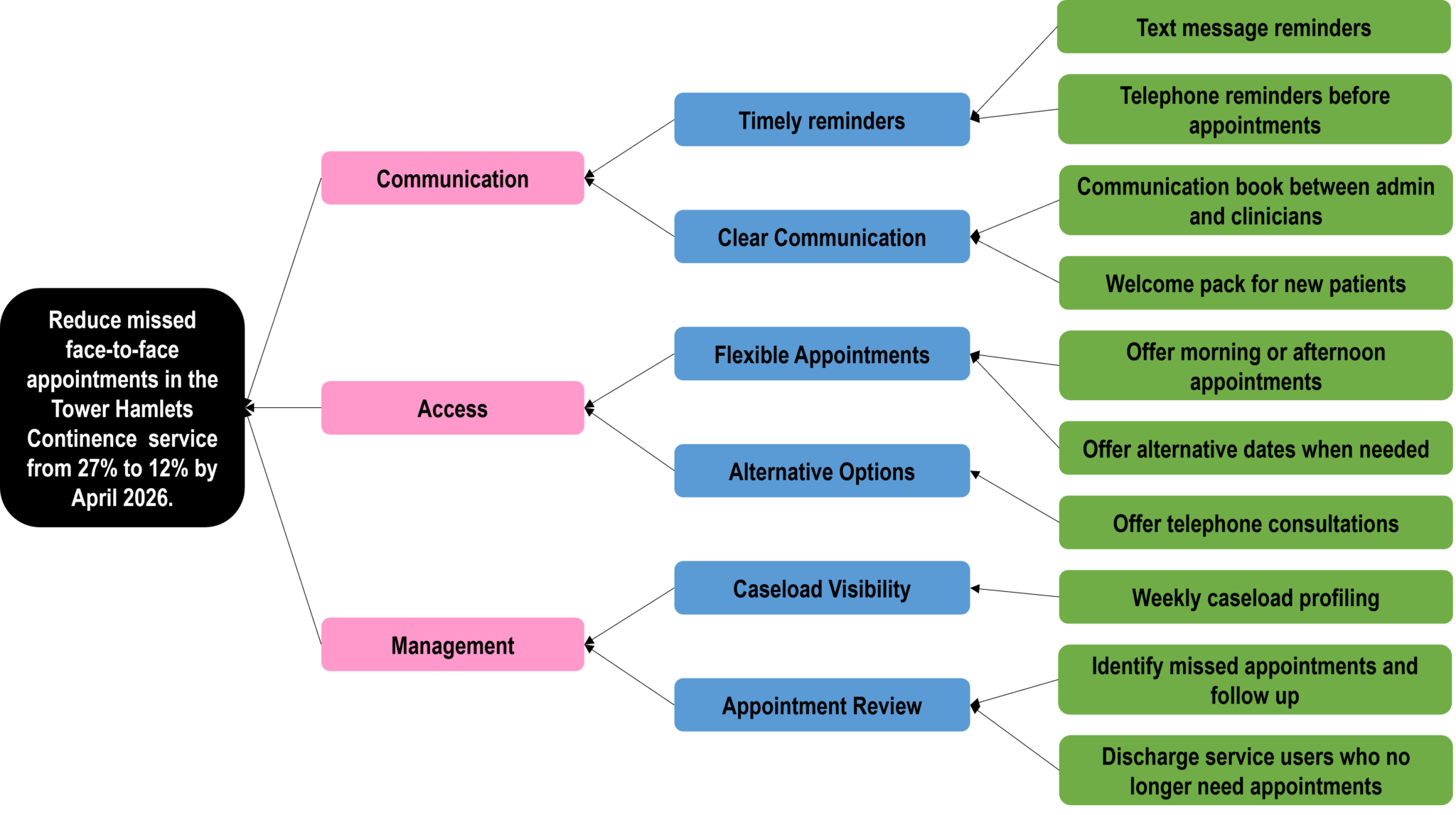
Using quality improvement methods, the team developed a driver diagram (Figure 1) to guide their approach and began testing changes through Plan–Do–Study–Act (PDSA) cycles.
Figure 1: The Tower Hamlets Continence Team Driver Diagram
Rather than introducing large-scale changes all at once, the team focused on small, meaningful adjustments. They began outreach sessions to educate local communities on continence and promote the service. They offered more flexible appointment times, giving service users greater choice and control. Communication was strengthened through a series of reminders, including text messages and phone calls at key points before the appointment. Where appropriate, telephone consultations were introduced, reducing the need for travel and making access easier.
At the same time, internal processes were improved. Weekly caseload reviews helped clinicians identify missed appointments, unnecessary follow-ups, and opportunities for discharge. Communication between administrative and clinical staff became more streamlined, ensuring that cancellations and re-bookings were managed quickly and efficiently.
Individually, these changes were simple. Together, they began to reshape how the service functioned.
What changed for service users and staff?
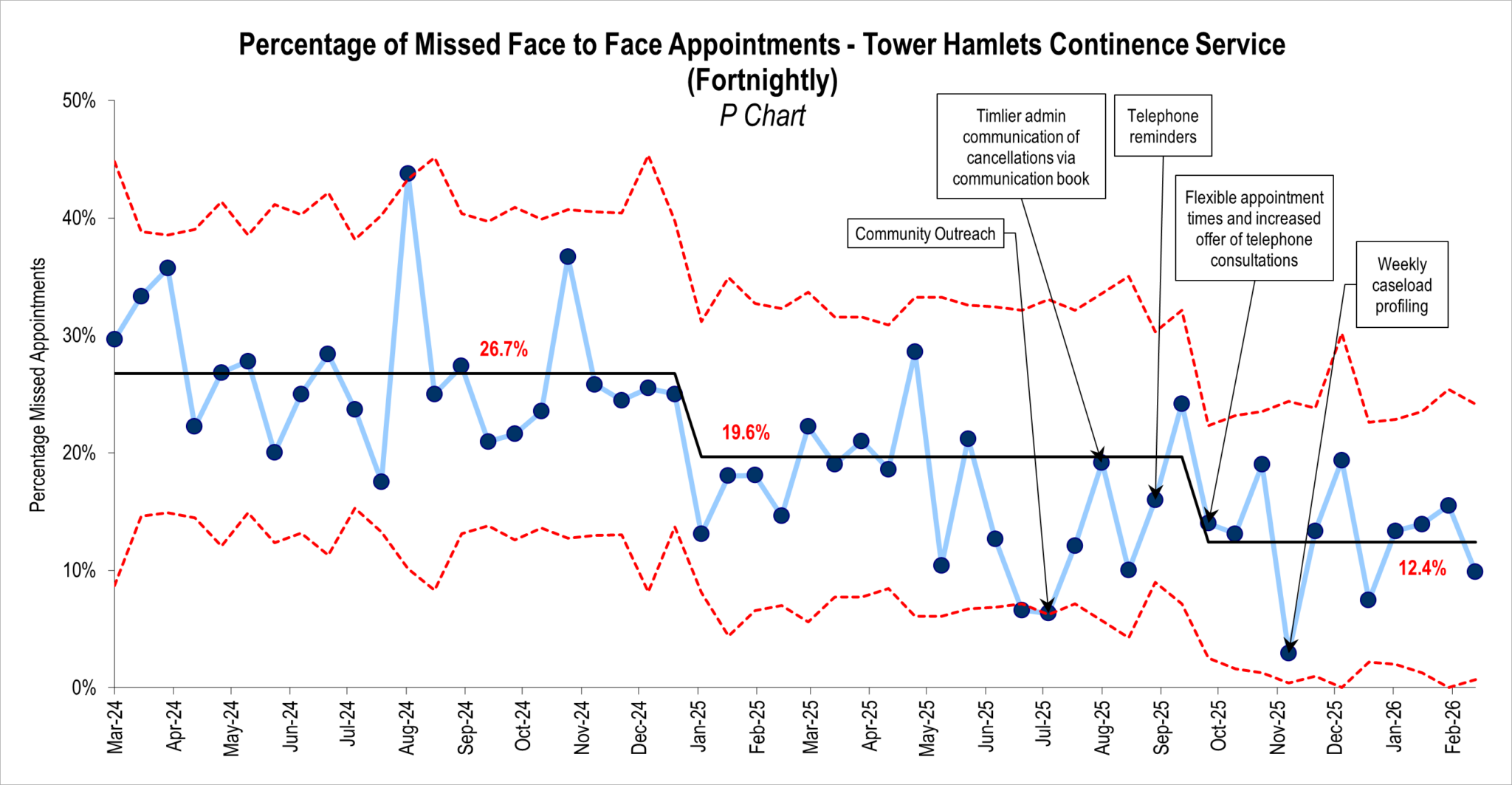
Over time, the impact became clear. The percentage of missed appointments reduced from 27% to 12%, meaning significantly more service users were able to access the care they needed (Figure 2).
Figure 2: Tower Hamlets continence service missed appointment percentage
Service users felt more involved and better supported, particularly when they could choose appointment times or opt for remote consultations. Reminder calls helped people stay on track, and clearer communication made it easier to reschedule when needed.
For staff, the changes led to better use of clinical time and fewer wasted appointments. The service shifted from being reactive to more proactive, with greater visibility of demand and capacity.
Perhaps most importantly, the team began to see a shift in mindset. Improving attendance was no longer about encouraging people to attend, it was about designing a service that made attendance possible.
What next for the project?
The team are now focused on ensuring that these changes are sustained and embedded. They are incorporating this approach into staff induction and training, and continuing to build it into everyday practice through regular team discussions, supervision, and feedback. The team are actively looking to share this learning more widely, supporting other services to reduce their own missed appointments. Alongside this, the team continue to strengthen collaboration with primary care, helping to promote health more effectively within the community.
Final reflections from the team
This work is a reminder that behind every missed appointment is a person, and behind every improvement is an opportunity to do better.
When we design services around people’s lives, not the other way around, we don’t just reduce missed appointments, we open the door to care, connection, and better outcomes for those who need it most.
Most Read Stories
-
Why is Quality Control important?
18th July 2018

-
2016 QI Conference Poster Presentations
22nd March 2016
-
Recognising Racism: Using QI to Help Take Action
21st January 2021

-
QI Essentials: What does a Chief Quality Officer do?
18th March 2019

-
Using data enabled us to understand our problem
31st March 2023

-

Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.