Cutting Waste, Boosting Care: How Newham’s Pharmacy Team is Reducing Medication Waste
8th April 2026
Written by Nate Addo (Clinical Lead Pharmacist), Veena Shivnath (Clinical Lead and Clozapine Pharmacist) and Clarissa Sørlie (Improvement Advisor)
The Problem: Medication Waste
Medication waste is a routine but often overlooked part of daily pharmacy work. It can arise from duplicated prescribing, changes in treatment, or medicines dispensed for inpatients that are no longer needed. Waste also arises from unused discharge or short-term leave medications, often due to delays or changes in discharge planning. Another key contributor is the limited reuse of medicines that could be safely reassessed and used, including patients’ own drugs.
When Clinical Lead Pharmacists Nate Addo and Veena Shivnath saw the volume of medication waste bins that were collected from wards and the dispensary, they knew that something needed to be done. Having recently started the Improvement Coaching Programme, Nate recognised the value of using a structured quality improvement (QI) approach to help the Newham pharmacy team to tackle the problem effectively.
A group of colleagues within the pharmacy team (see image 1 below) assembled to form a QI project team, with the aim of reducing medication waste in the Newham Centre for Mental Health Pharmacy Department by 50% by July 2026. A member of the team registered for the Improvement Leaders Programme to support delivery of the project.

Image 1. Some of the project team members (left to right: Nate Addo, Aisha Mulla, Veena Shivnath, Mohammed Rashid, and Riyah Hossain). Colleagues not pictured: Ann Anosike and Shohaib Ahmed
The Tests That Are Making a Difference
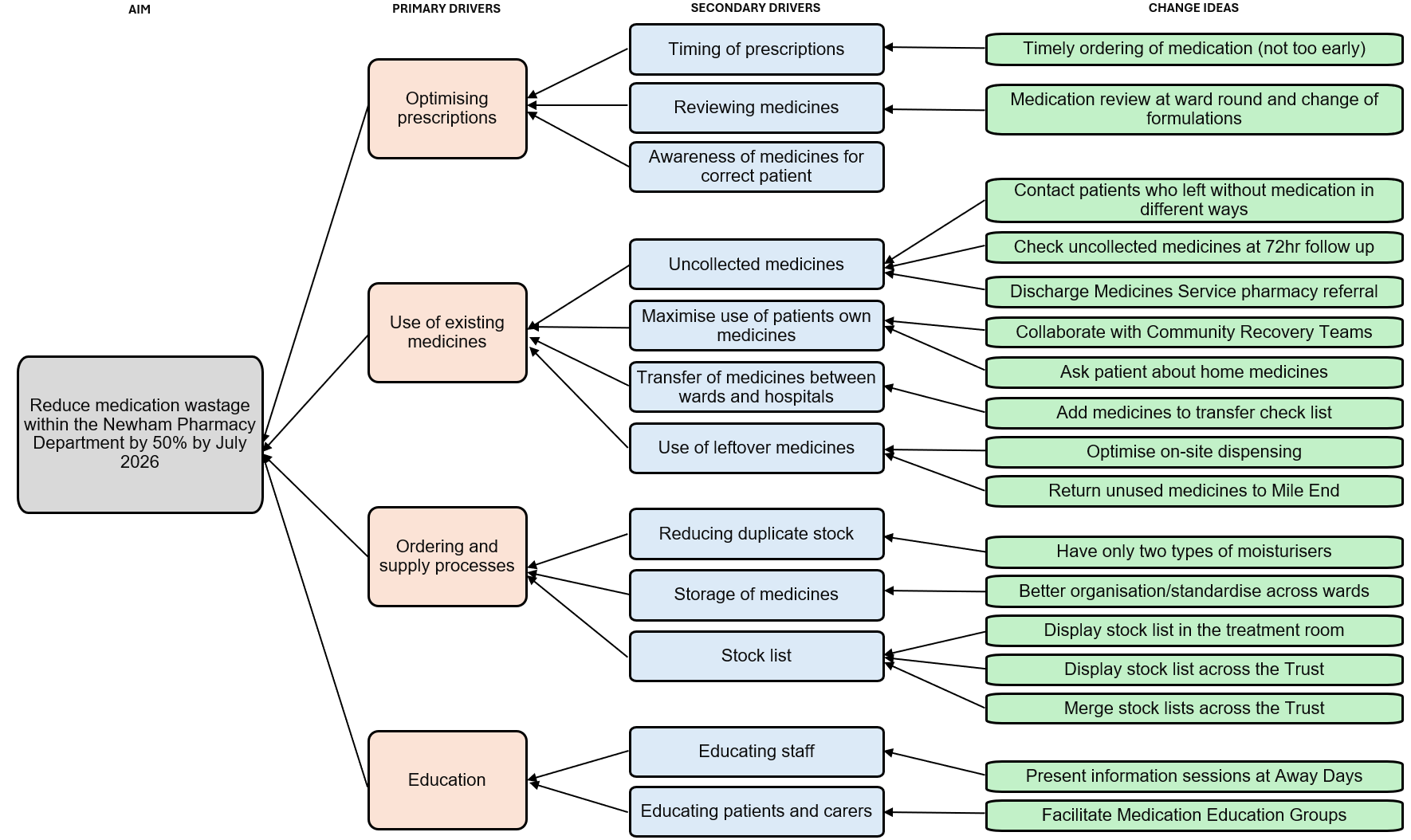
The team have displayed their change ideas visually using a driver diagram (see image 2).
Image 2. The team’s change ideas represented visually on a driver diagram
So far, they have tested three ideas that are showing promise:
- Increasing safe return and reuse of medication: Ward medications were systematically returned and reused, enabling safe reuse of medications that would otherwise have been wasted. The team estimate that this test produced a cost saving of £8k.
- Tightening collaboration with Community Recovery Teams: The teams worked more closely with Community Recovery Teams to bring in depot when patients are admitted. The team estimate that this intervention has delivered savings of almost £4k, while preventing unnecessary duplication of ordering. Importantly, it has also reduced delays to care and minimised the risk of depot medications, often administered every three months being wasted or expiring during inpatient stays.
- Optimising on-site dispensing: Using inpatient supplies and patients’ own drugs to fulfil medications for short term leave or discharge. This has not only reduced medication waste (estimated saving of £1k) but has helped the discharge process, reducing delays and improving the overall patient experience.
Collectively, these relatively small but strategic changes have demonstrated how focused, system-wide interventions can deliver meaningful improvements in efficiency, cost savings, and patient care.
The Impact for People, Pounds and Planet
Reducing waste directly improves patient care, while also providing financial savings and reducing environmental impact.
- People: Better Care Through Smarter Systems
Reducing medication waste directly benefits patient care, safety, and experience. Financial savings can be reinvested into frontline services, while process improvements enhance efficiency.
For example, introducing onsite dispensing has reduced waiting times for discharge medication, improving patient experience. Collaborating with community teams to utilise existing depot medications has not only saved money but also prevented delays in treatment. Including medication checks in 72-hour post-discharge follow-ups ensures any issues are identified and escalated promptly.
Simple prescribing improvements also make a difference. Encouraging prescribers to know the appropriate strengths and formulation, for instance, prescribing one 400mg tablet instead of two 200mg tablets, reduces tablet burden, improves adherence, and supports better patient outcomes.
- Pounds: Small Changes, Big Savings
Medication waste is a significant issue at both local and national levels. The UK government estimates that around £300 million is wasted each year due to unused medicines across the NHS (Department of Health and Social Care, 2011; Smith, 2026), highlighting the scale of the opportunity for improvement.
The team are collecting detailed data on the cost of every medication and have estimated the following savings to date since July 2025, based on costings from the NHS Drug Tariff. These figures will be formally calculated and evaluated at the end of the project:
- Total savings: £12,923
- Savings from safe return and reuse of medication: £8,035
- Savings from collaboration with Community Recovery Teams: £3,926
- Savings from on-site dispensing: £962
- Planet: Cutting Carbon by Reducing Waste
Environmentally, wasted medicines contribute to carbon emissions at every stage – production, transport, and disposal. Incineration releases greenhouse gases, while improper disposal can lead to water pollution and antimicrobial resistance. Packaging waste adds further impact. According to NHS England (2026), medicines contribute a quarter of carbon emissions within the NHS in England, meaning that waste reduction is essential to achieving Net Zero targets.
The team are routinely collecting data on their tests of change, to support an evaluation of the environmental impact at the end of the project.
Lessons from the Project
The team’s key insight: “problems which initially feel overwhelming become much more manageable when approached systematically”.
They learned that:
- Root causes of medication waste are unearthed by applying QI tools
- Using a structured methodology creates clarity from complexity
- Working collaboratively to identify solutions make the challenge feel less daunting
What’s Next?
The team will continue to test a range of change ideas, including reviewing ward stock lists, trialling a standardised medication transfer checklist between wards, and exploring how the Discharge Medicines Service can better support continuity of care and reduce waste. Additional focus will be placed on optimising medication storage practices to minimise avoidable losses.
Alongside testing, there will be an emphasis on embedding successful interventions into routine practice, strengthening multidisciplinary engagement, and improving data collection to track impact more robustly. Sharing learning across teams and spreading effective changes across the organisation will be key to achieving sustained reduction in medication waste.
References:
Department of Health and Social Care (2011) Action on Medication Wastage and Improving Medicine Use [Online]. Available at: https://www.gov.uk/government/news/action-on-medicine-wastage-and-improving-medicine-use (Accessed: 31st March 2026)
NHS England (2026) Delivering a Net Zero NHS: Areas of Focus [Online]. Available at: https://www.england.nhs.uk/greenernhs/a-net-zero-nhs/areas-of-focus/ (Accessed: 31st March 2026)
Smith, M. (2025) ‘Reusing Medications to Mitigate Their Environmental Impact’, Prescriber, 5, pp. 5-8 [Online]. DOI: 10.1002/psb.2124 (Accessed: 31st March 2026)
Most Read Stories
-
Why is Quality Control important?
18th July 2018

-
2016 QI Conference Poster Presentations
22nd March 2016
-
Recognising Racism: Using QI to Help Take Action
21st January 2021

-
QI Essentials: What does a Chief Quality Officer do?
18th March 2019

-
Using data enabled us to understand our problem
31st March 2023

-

Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.