How Rethinking Baby Observations Improved Quality and Reduced Costs on the East London Mother and Baby Unit
12th January 2026
Written by Catherine Furlonge (Lead Nursery Nurse) and Clarissa Sørlie (Improvement Advisor)
Background
In early 2024, the East London Mother and Baby Unit (MBU) faced a growing challenge: an increasing number of babies were placed on enhanced observations, particularly at night. At times, up to nine babies required one-to-one observations, meaning nine staff members were needed for observations alone. This model was unsustainable, leading to:
- Heavy reliance on bank healthcare assistants
- Increased staffing costs
- A crowded ward environment
- Reduced independence and confidence for patients

Figure 1. A baby enjoying the Mother and Baby Unit sensory room (photograph used with parental consent).
Recognising the opportunity to improve these issues, the team launched a Quality Improvement (QI) project to redesign observation practices without compromising safety or quality.
Change Ideas
Zonal Observation Model
The ward was divided into zones with one staff member responsible for up to three babies, improving efficiency while maintaining close supervision and support. This model had previously been tested at scale as part of a Trust-wide programme to improve observation practice (Aurelio et al., 2025).
Colour-Coded Observation System
A colour-coded visual system was introduced to clarify observation levels:
- Red: One-to-one, arm’s length support
- Orange: One-to-one, within eyesight
- Yellow: Check-ins every 15 minutes
- Green: Check-ins every 30 minutes
This system was displayed in patient rooms (see Figure 2) and explained at admission, improving transparency and understanding.
Figure 2. Colour-coded observation guides displayed in patient bedrooms for transparency and peace of mind
Ward Activities
Team members undertook training which enabled them to offer baby yoga as a regular activity on the ward. This, along with other activities such as baby massage, improved meaningful engagement for patients and enhanced the ward atmosphere.
Figure 3. A varied timetable showcasing baby yoga, massage and other therapeutic activities
Project Impact
Ward Improvements
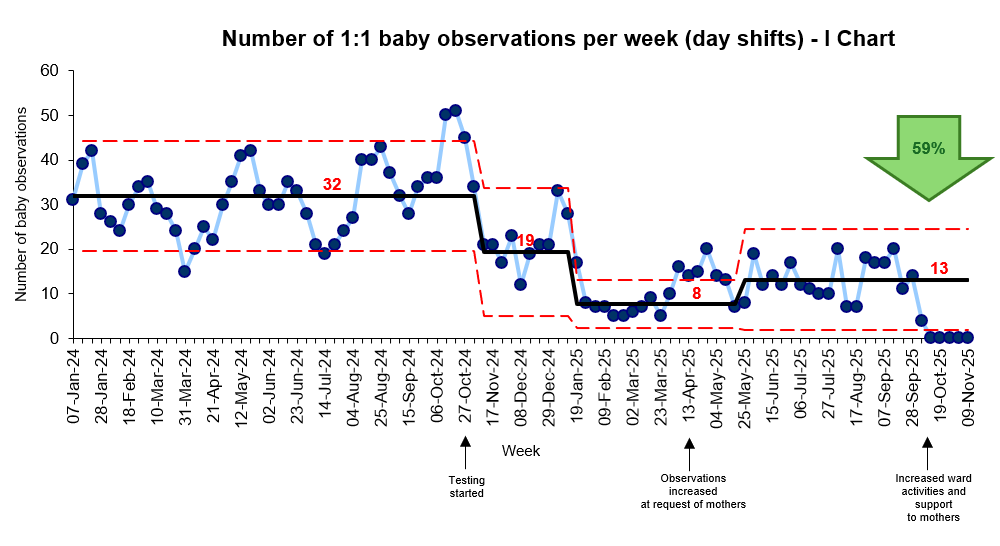
- Daytime enhanced observations reduced by over half (59%) – see Figure 4
- Night-time observations reduced by a third (39%)
- Staffing stabilised from up to nine staff at night to a consistent six across shifts (saving three staff per night shift)
- The safety of patients and their babies was maintained
- The ward environment felt calmer and more therapeutic
Figure 4. Daytime one-to-one baby observations reduced by more than half, creating a calmer ward environment
Staff and Patient Experience
- Staff reported feeling less stressed
- Patients gave positive feedback, including one ex-patient who shared:
“I came to visit a patient on the ward last night and just wanted to give you some feedback on the traffic light levels of care.
The mother asked me how it will work when her baby arrives, and I was able to point her to the lovely posters on the wall and reassure her that she is in the best hands and when her baby comes, he’ll be in good hands too. She had some anxiety around needing to sleep and wanting to be with her baby, and it was all so clear from the posters how it will work.”
Financial Impact
- Bank staff costs reduced by a third (see Figure 5)
- Average monthly savings of approximately £22,241, equating to an estimated £266,892 annual saving
- Reduced reliance on temporary staff improved continuity of care
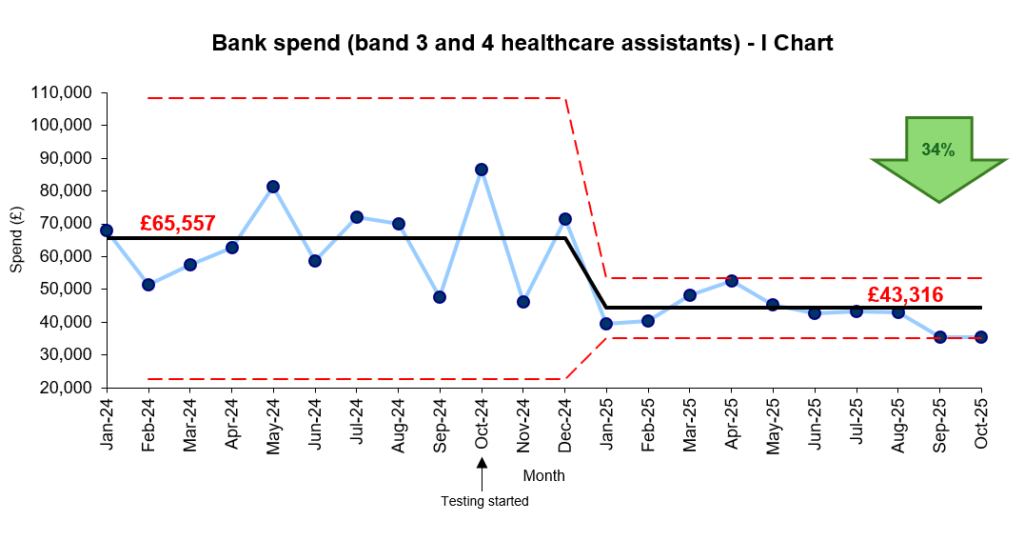 Figure 5. Bank staff costs reduced by 34%, freeing resources for better patient care
Figure 5. Bank staff costs reduced by 34%, freeing resources for better patient care
Reflecting on the impact of the project, Deputy Clinical Director Victoria Cohen said, “The changes the team have made to the patient and baby care on MBU are impressive and a testament to the care they show for the patients and the service.”
Lessons Learned
- Aligning observation levels with actual clinical need improves patient experience while maintaining safety
- Visual tools (colour-coded system) enhance clarity for staff and patients
- When care models prioritise empowerment and efficiency, financial savings follow
Conclusion
This project showed that meaningful change happens when safety, empowerment, and efficiency align. By rethinking observation practices, the team not only created a calmer, more therapeutic environment for patients and staff but also delivered measurable financial savings and operational stability. Reducing unnecessary one-to-one observations cut costs by a third – resources that can now be reinvested in patient care. Most importantly, patients felt more confident in caring for their babies, and staff regained control of their workload. This is a clear example of how improving experience and quality drives sustainability.

Figure 6. Catherine, the project lead, standing outside the Mother and Baby Unit
References
Aurelio, M., Singh, S., Chitewe, A., Mckenna, C., Marufu, E., Bridle, D., Sunduza, L. and Shah, A. (2025) ‘Improving therapeutic engagement and observations on inpatient mental health wards in the English National Health Service: lessons from using quality improvement to scale up interventions’, International Journal for Quality in Health Care, 37(3), pp. 1-9. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12380470/ (Accessed: 23 December 2025)
Most Read Stories
-
Why is Quality Control important?
18th July 2018

-
2016 QI Conference Poster Presentations
22nd March 2016
-
Recognising Racism: Using QI to Help Take Action
21st January 2021

-
QI Essentials: What does a Chief Quality Officer do?
18th March 2019

-
Using data enabled us to understand our problem
31st March 2023

-

Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.