Improving Physical Health in Tower Hamlets Early Intervention Service
20th January 2026
Written by Vernanda Julien (Improvement Advisor)
Figure 1. Physical Health Notice Board
Background
Tower Hamlets Early Intervention Service (THEIS) launched a Quality Improvement (QI) project in March 2023 to address a critical gap in physical health care for service users. At the start of the project, only 28% of annual physical health assessments were fully complete, which was below the national Early Intervention target of 90%.
Adults with psychosis or schizophrenia have a life expectancy 15 to 20 years shorter than the general population (NICE QS80). Comprehensive physical health checks are essential to identify risks early and offer timely interventions. THEIS recognised that improving these checks wasn’t just about meeting target, it was about improving lives.
A project team was formed consisting of Matthew Bacon (Senior Nurse Practitioner), Aaron Frazer (Care Coordinator/Social Worker), Sarah Payne (Senior Practitioner/Mental Health Nurse) and Dalila Magdu (Improvement Coach/Quality Improvement & Clinical Governance Coordinator)
What Was the Problem?
In order to address the gap in the completion of physical health assessments, the team needed to address two key areas:
- Assessment – What was the process for offering and completing all required checks?
- Intervention – How was appropriate support offered and recorded?
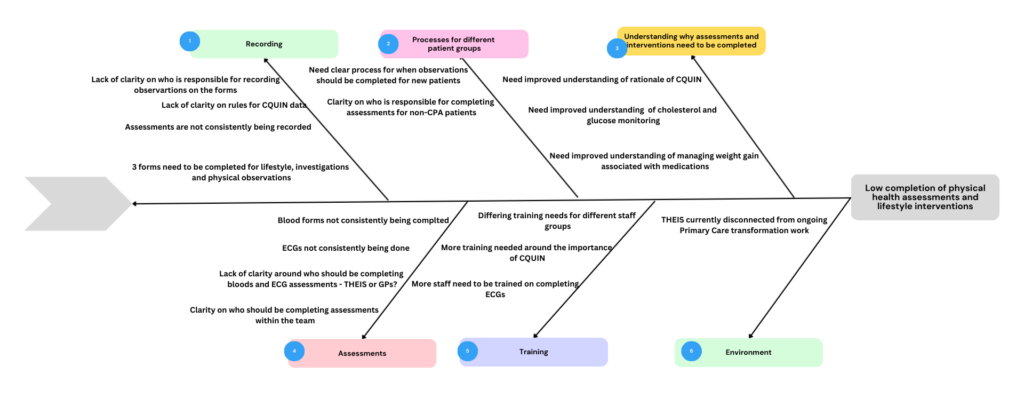
In order to understand the problem, the team utilised a fishbone diagram (Figure 2) to explore barriers such as unclear roles, inconsistent recording, and gaps in training.
Figure 2. Fishbone Diagram exploring the problem with assessing physical health
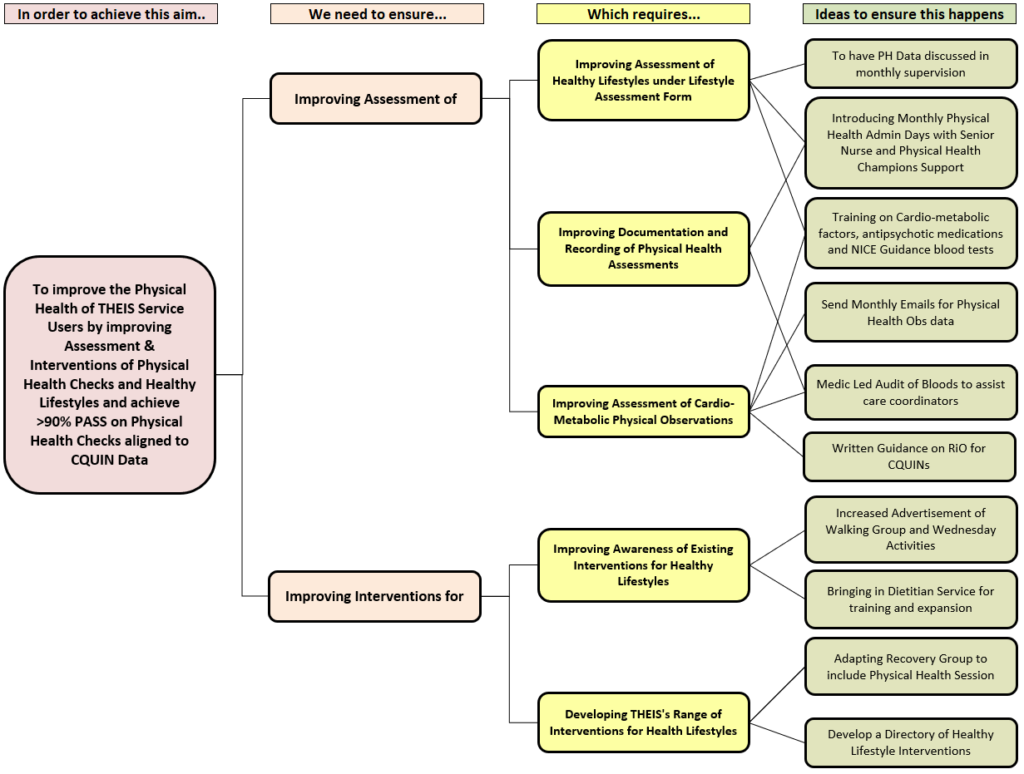
Focus groups were held with service users which provided insights into the barriers to having physical health checks completed and also suggestions of change ideas. Once the team had a better understanding of the problem, a driver diagram (Figure 3) was developed to map out the change ideas they could test to improve the completion of physical health assessments.
Figure 3. Driver Diagram – Improving the physical health of THEIS service users
What Did They Do?
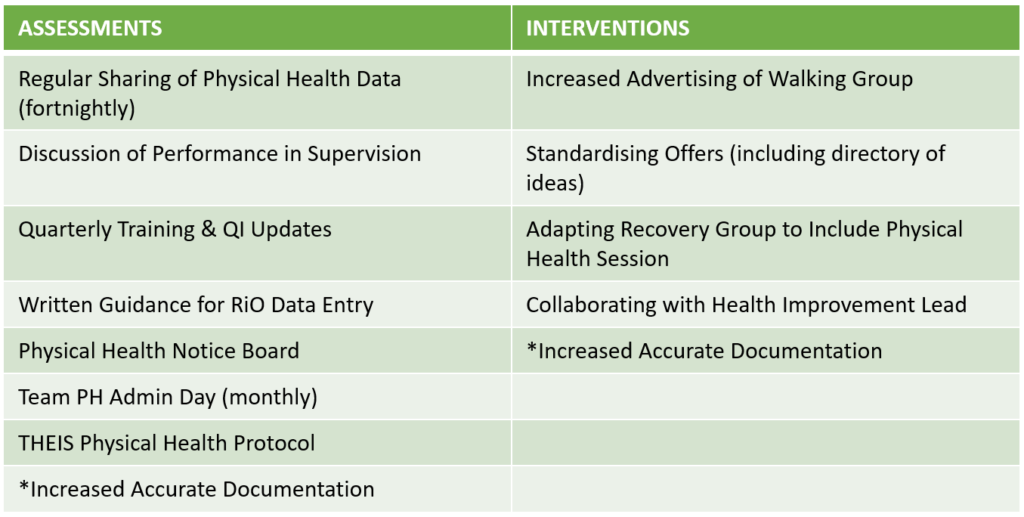
The team tested several change ideas to address the challenges around completing physical health assessments and offering lifestyle interventions (Table 1).
Table 1. Change ideas tested by THEIS
The change ideas which had the biggest impact were:
- Monthly physical health admin days where senior nurses and physical health champions supported care coordinators with reviewing the physical health entries for their caseloads and understanding CQUIN data.
- A quick guide to physical health CQUIN assessment and documentation which gave step by step instructions on how to accurately input physical health assessments on the clinical system RiO and the steps to take if interventions were required.
- A physical health notice board and simplified physical health protocol (Figure 1) which drew on guidance and evidence from ELFT, NICE, and RCPSYCH. This ensured staff and service users had easy access to the relevant information and helped to ensure processes around physical health assessments monitoring and interventions are simple and appropriate.
What Difference Did It Make?
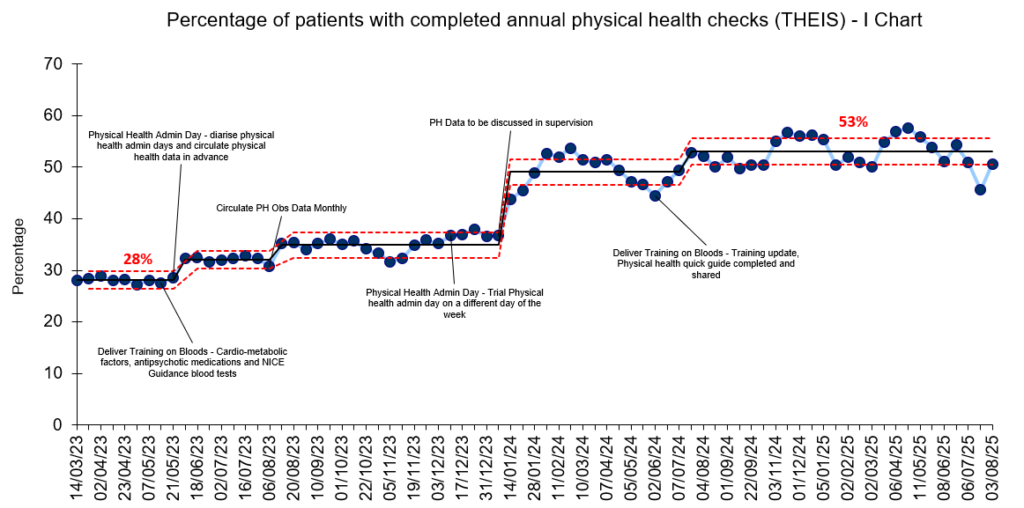
To monitor the impact of their change ideas, the team collected data on the percentage of patients with completed annual physical health checks (Figure 4) and percentage of patients who accepted required interventions (Figure 5) as outcome measures.
Figure 4. I chart showing percentage of patients with completed annual physical health checks
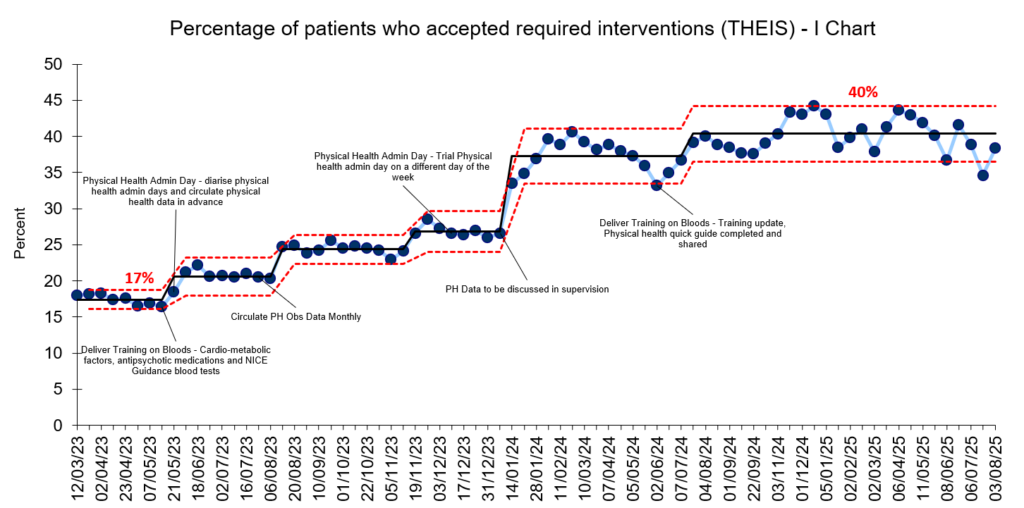
Figure 5. I Chart showing the percentage of patients who accepted required interventions
The team saw sustained improvements in both of their outcome measures with an increase in the percentage of completed physical checks from 28% to 53% and an increase in the percentage intervention being accepted from 17% to 40%.
What’s Next?
As the project came to an end, Matthew Bacon, Senior Nurse Practitioner, reflected, “This project wasn’t just about hitting numbers, it was about creating a culture where physical health is everyone’s business.”
The team has developed structured processes like monthly admin days, local protocols, and embedding discussions into MDT meetings which will enable them to sustain their improvements. They intend to:
- Continue quarterly physical health training
- Bring physical health data into monthly multidisciplinary team meetings to enable regular data reviews.
- Continue performance discussions in supervision.
- Appoint a physical health lead who will have oversight over the physical health monitoring in the team
- Employ a physical health assistant or support worker
- Most importantly – Keep patients healthy!
Most Read Stories
-
Why is Quality Control important?
18th July 2018

-
2016 QI Conference Poster Presentations
22nd March 2016
-
Recognising Racism: Using QI to Help Take Action
21st January 2021

-
QI Essentials: What does a Chief Quality Officer do?
18th March 2019

-
Using data enabled us to understand our problem
31st March 2023

-

Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.