Managing confidence in physical health emergencies on inpatient psychiatric wards
9th April 2026
Our QI journey through the Improvement Leaders Programme (ILP): McPHEW (Managing confidence in physical health emergencies on inpatient psychiatric wards)
Written by Hester Mannion, Rohan Krishnan, Sushmita Sidhu, Daniel Turton, Ali Iqbal, Tania Rahman, Rachel Darracott-Cankovic, Aira Manguiat (QI coach), Matt Oultram (Improvement Advisor)
Resident doctors providing ward cover in psychiatric inpatient settings often face the challenge of managing urgent physical health issues out of hours with limited support, contributing to stress, uncertainty, and avoidable transfers to A&E. In response to this and motivated by the frustrations we have experienced working these shifts, we devised a QI project to improve confidence, morale, and access to guidance for clinicians, with the overall aim of enhancing patient safety.
We took the opportunity to bring our project to Cohort 15 of the Improvement Leaders Programme (ILP) which started in November 2025. This provided us with a fun and collaborative space to learn QI methods and skills together, to develop our project and network in-person. Joining ILP marked a real turning point for our project, giving us the momentum and skills we needed to take it to the next level.
Learning about the problem
Early surveys highlighted several key concerns: difficulty accessing senior advice, inconsistent communication with acute teams, limited access to investigations, and lack of confidence in tackling complex or ambiguous presentations. Doctors also described challenges with handovers, variable nursing support, and outdated knowledge of clinical guidelines. These insights shaped a series of practical interventions.
Our theory of change
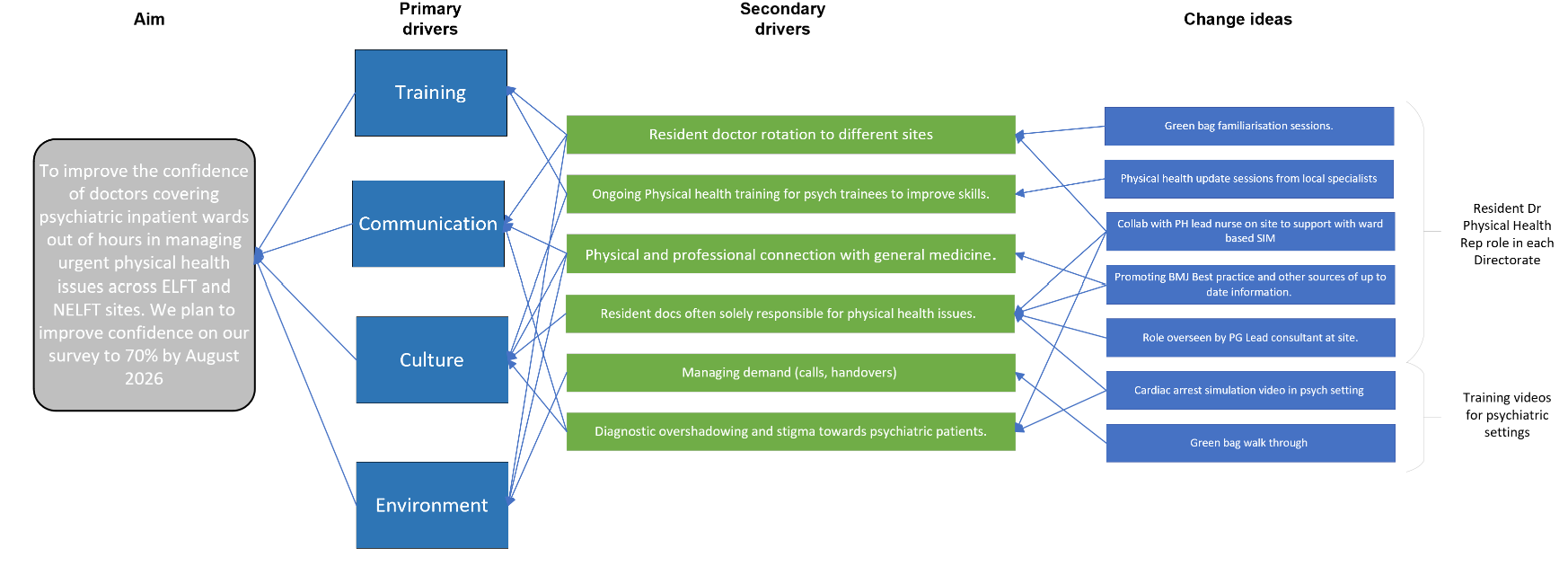
Following our engagement with resident doctors we developed the following driver diagram (Fig. 1)
Here we have set out what we think will contribute significantly to improving confidence, such as improving training, communication between staff and services and familiarization with emergency procedures.
Fig 1. Driver Diagram
Change ideas
Our change ideas included strengthening links with local acute medical teams, working with locality physical health lead nurses to collaborate with ward based simulation, emergency grab‑bag familiarisation and academic updates on physical health. One of our most successful change ideas has been our development of the role of ‘physical health representative’, held by a resident doctor for six months devised to support their peers to access training and skills for the management of physical health.
Our video
A major change that is currently in progress is our educational video. This video, currently in post-production, was shot by a professional media company and included medical, operational staff and service users. Below is a screenshot (Fig.2) from our draft recording, but please watch this space for the final result! Our service user representative Rachel, has supported us significantly with developing and carrying out this test.

Figure 2. Screenshot from draft recording of our training video
As the project has evolved, it has expanded across boroughs and introduced new structures like the six‑monthly Physical Health Representatives to maintain momentum.
How are we measuring our progress?
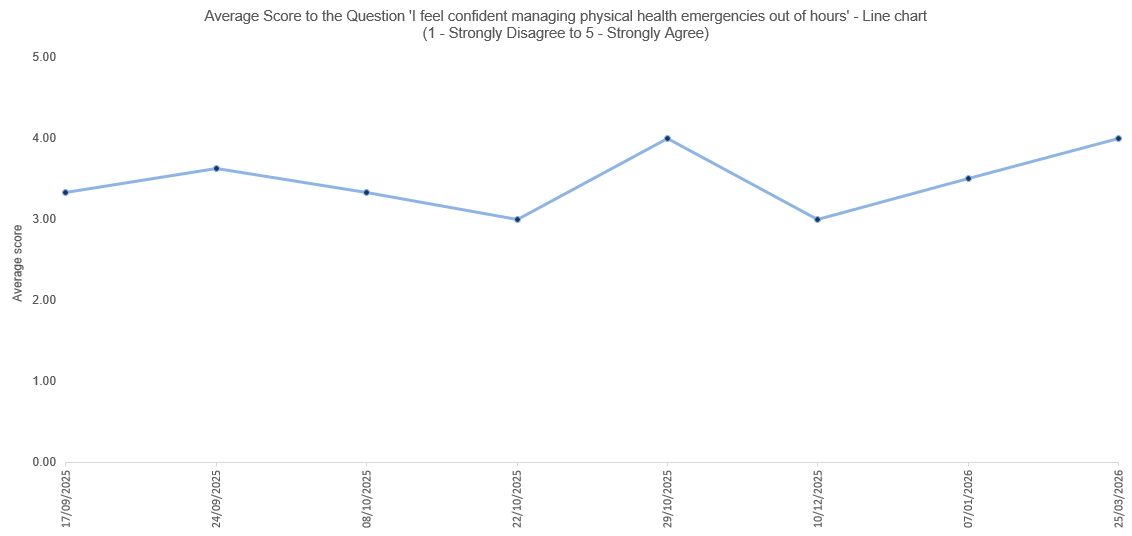
Figure 3. Confidence in managing physical health emergencies
Our outcome measure (the measure directly related to our aim statement) focuses level of confidence around managing physical health emergencies. This is tracked by through a regular survey completed by our physical health reps, and is plotted on the run-chart above (Figure 3). We would like to increase this number to a score of 4 by August 2026.
Alongside this data, we also collect views of resident doctors. This gives us valuable insight into their experiences and has included the following –
“The inclusion of physical health teachings on Wednesday have increased the knowledge and improved communication and networking with the main hospital.”
“Knowing there is a PRU team I can speak to besides the med reg has been useful”.
“Very useful to see green emergency bag. Video introduction is a very good resource”.
Going forward
As we near the end of the Improvement Leaders Programme, we have seen the project develop into a trust-wide initiative, involving service users and colleagues from across services, overcoming numerous obstacles and managing a project alongside demanding workloads and responsibilities.
The team now looks toward sustaining progress, deepening cross‑team relationships, continuing the successful extension of the project in our sister-trust NELFT—building a more supportive and confident out‑of‑hours workforce for safer inpatient care.
Most Read Stories
-
Why is Quality Control important?
18th July 2018

-
2016 QI Conference Poster Presentations
22nd March 2016
-
Recognising Racism: Using QI to Help Take Action
21st January 2021

-
QI Essentials: What does a Chief Quality Officer do?
18th March 2019

-
Using data enabled us to understand our problem
31st March 2023

-

Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.