Reducing administrative errors in the Bedford and Luton Psychiatric Liaison Service (PLS) and Crisis Teams
23rd January 2026
Project Team: Michelle Woodward, Alison Robertson, William Adkins, Susan Macauley, and Robin Beales
QI coach: Stuart Williams
Improvement Advisors: Miles Tringham & Cassie Philpin
Background
Incorrect data being entered onto RiO, has a negative impact on staff and services. This means that staff must spend time correcting mistakes, leading to teams not having the most accurate information regarding their caseloads.
To improve the efficiency of their services, the admin team in Bedford and Luton PLS and Crisis Teams have been working to reduce the number of administrative errors being made.
Understanding the problem
The team started to collect baseline data to help them understand the frequency of administrative errors being made, with an average of 35 per week in the Psychiatric Liaison Service (PLS) and 83 per week in the Crisis Team.
They reviewed the most common administration errors and identified the following
- DISCHARGE
- Discharge destination
- Time and date of discharge
- REFERRAL
- Time and date of referral
- Referral source
- Status (emergency urgent / 24 hour)
- Health Care Professional allocation
- DIARY MANAGEMENT
- Appointments not entered
- Incorrect time and/or date
- Outcomes not updated
The root cause of administrative errors identified by the team was a lack of knowledge of how to correctly update the RiO patient notes system, which is not always an intuitive one.
Developing a theory of change
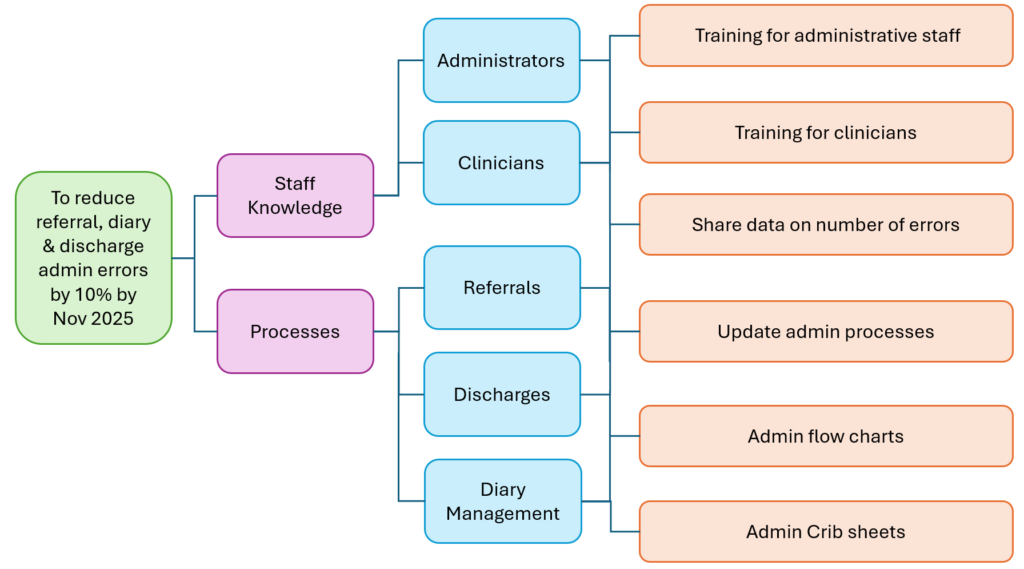
The team developed a Driver Diagram (see Figure 1) to capture their theory about what changes needed to be introduced to help them achieve their aim of reducing administrative errors by 10% by November 2025.
Figure 1: Driver Diagram
Testing change ideas
The team used Plan Do Study Act cycles, and an iterative process of introducing change ideas, reviewing their data and getting feedback from the QI project team during catch ups.
- Change idea 1: Training for team administrators
- Training was delivered in January 2025
- Staff reported that the training was helpful, but data did not demonstrate any improvement.
- Admin staff felt that it would be helpful to have updated procedures and crib sheets that they could refer to after the training and that clinical staff needed to be informed of admin processes too.
- Change idea 2: Crib sheets circulated to admin and clinical staff
- Crib sheets with step-by-step admin instructions were created, saved in designated folders, and circulated to all staff in April 2025
- The introduction of this change resulted in a reduction in errors in the Crisis Team.
- Change idea 3: Training for clinical staff
- Training for clinical staff was delivered in both a team environment as well as one-to-one sessions in July 2025.
- The combination of sharing crib sheets and training to both clinical and administrative staff helped achieve a reduction in errors in both teams.
Data
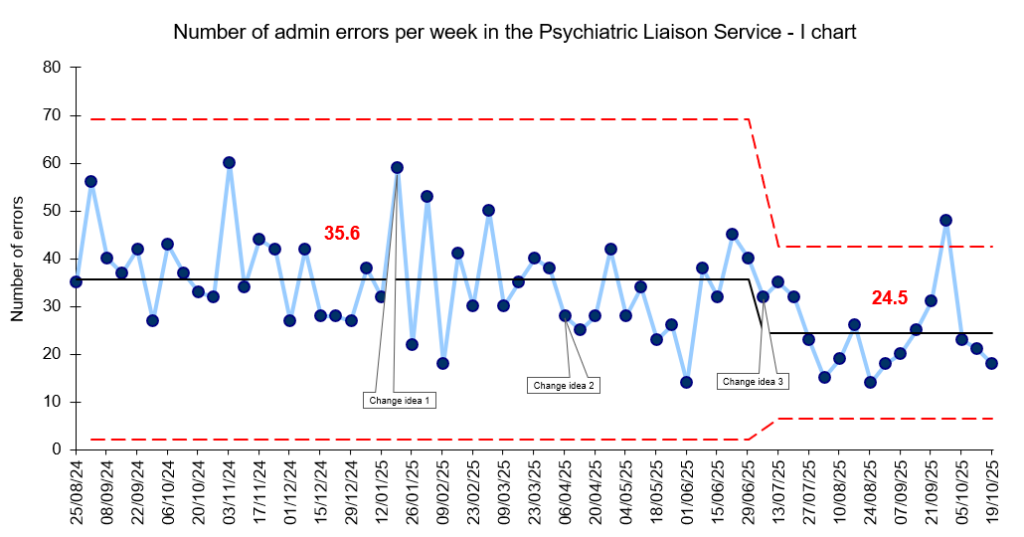
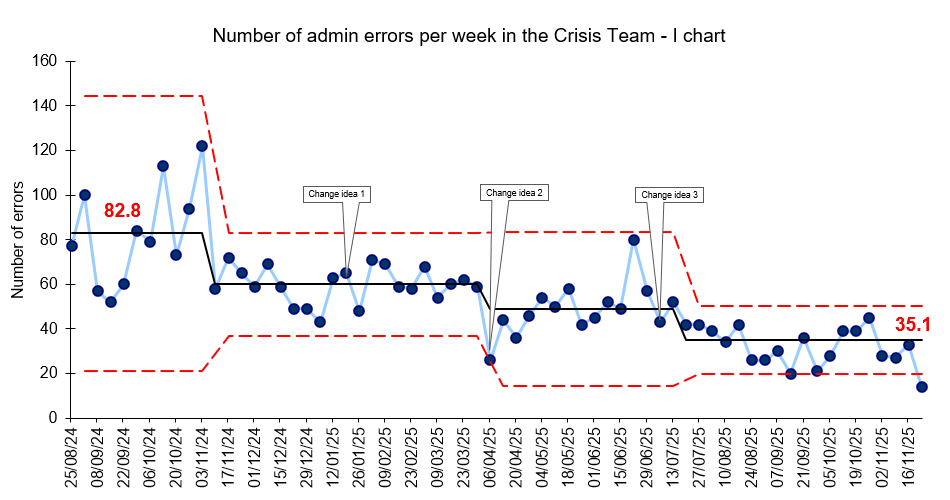
Both teams exceeded their goal, with the PLS achieving a 31% reduction in errors (Figure 2), and the Crisis Teams seeing a 58% reduction in administrative errors (Figure 3).
Figure 2: Number of admin errors per week (PLS)
Figure 3: Number of admin errors per week (Crisis Teams)
The importance of Human Factors in QI
The learning from this project; that training alone does not lead to improvement, reflects the finding of many patient safety studies. While education is likely to be a necessary component of a change package when a lack of knowledge has been identified as a contributing factor (as was the case in this project), it cannot solely be relied upon to achieve behaviour change.
Human factors reminds us that most errors in healthcare are generally not caused by a lack of knowledge, but how systems, environments, and workflows shape human behaviour. People forget things, get distracted, work under pressure, and adapt to poorly designed processes. Sustainable improvement therefore comes from redesigning work to make doing the right thing easier.
In this project, to supplement the training, the creation of crib sheets with step-by-step instructions for staff to refer to means they no longer must rely on memory to get things right.
Impact
By reducing errors, the admin team have helped to ensure clinical staff have access to the correct patient information, that patients receive the correct appointments, and that senior managers have accurate statistics regarding service utilisation.
The administration team estimates that each error takes approximately five minutes to correct. Before the project began, the two teams were averaging 119 errors per week, meaning administrative staff were spending nearly 10 hours each week on corrections. By reducing errors to an average of 59 per week, the team has halved the time spent on administrative re-work; freeing up the equivalent of 34 working days per year to focus on higher-value activities.
Implementation
To ensure the improvements are maintained, the team have a plan for embedding their change ideas:
- Training will be part of admin inductions
- Training will be offered as required, to clinicians to account for staff turnover
- Crib sheets will be reviewed, updated and circulated annually
- Data on the number of errors will be reviewed quarterly in MDT team meetings to maintain awareness of the issue.
After presenting their improvement work at the Beds & Luton Community QI Forum, it was agreed that the project had been a success and if similar issues were to arise in other teams, skills learnt throughout this project could be shared.
Most Read Stories
-
Why is Quality Control important?
18th July 2018

-
2016 QI Conference Poster Presentations
22nd March 2016
-
Recognising Racism: Using QI to Help Take Action
21st January 2021

-
QI Essentials: What does a Chief Quality Officer do?
18th March 2019

-
Using data enabled us to understand our problem
31st March 2023

-

Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.