Pursuing Equity
What is health equity?
Equity is one of the core aims of improving quality (2021, Institute of Medicine).

Equity in healthcare is described as “Absence of unfair, avoidable or remediable differences among groups of people, whether those groups are defined socially, economically, demographically, or geographically or by other dimensions of inequality.”
(World Health Organisation)
Equity differs from equality, which sees everyone treated the same irrespective of their circumstances. You can see this difference in the illustration.
Featured Article
Supporting teams to pursue equity
In response to the trust strategy to improve quality of life for all we serve, the trust launched a Quality Improvement (QI) programme to support teams to pursue equity.
Phase one
The programme began in April 2022 and was designed in partnership with colleagues from public health, people participation, the trust’s networks, and the QI department.
The programme brought together 14 teams from across the trust, to support them to use QI to improve equity in their local areas. Topics that were tackled included

Across the programme 71% of teams tested at least one change idea and over 20 change ideas were tested in total, including but not limited to:
- Staff training around race
- Offering self-bookings, drop-in clinics and weekend appointments
- Women’s groups to talk about sexual issues on forensic inpatient wards
- Family interventions
- Promoting services via barbers, gyms and social media to increase referrals from minority groups
- Redesigning clinical systems such as RiO to include screening status
- Recruitment videos
These change ideas resulted in 30% of teams seeing an improvement in their outcome measure, with 15% of teams also seeing an improvement in one of their process measures. See below for some of our most impactful results.
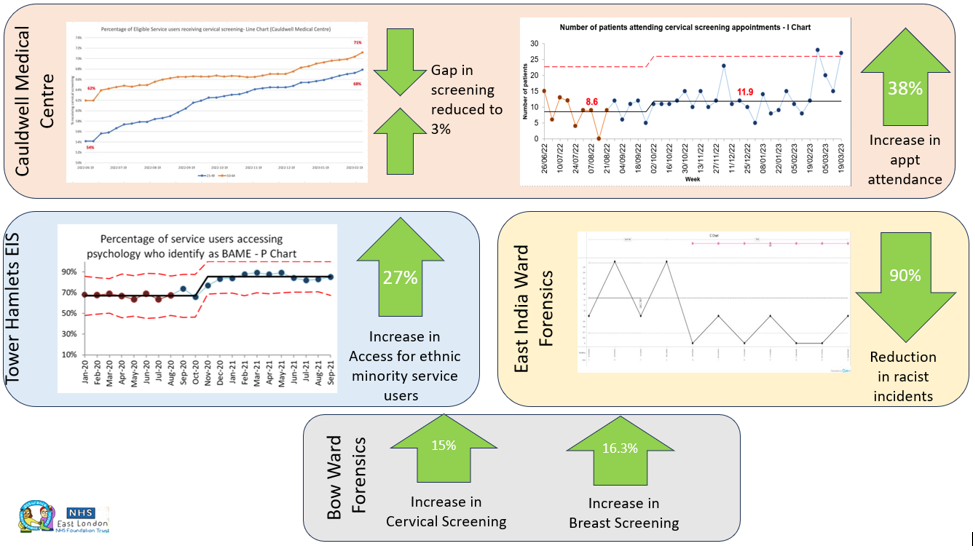
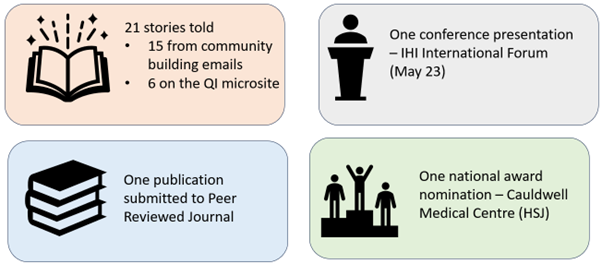
The wider impact of the work reached far and wide, including:
Phase two
The second phase of the programme began in September 2023 and built on the success of phase one to support teams to use QI to tackle inequity.
21 teams came together and used QI methods to tackle a wide range of equity issues that were most important to the teams and the populations they serve. Some examples of the work included:
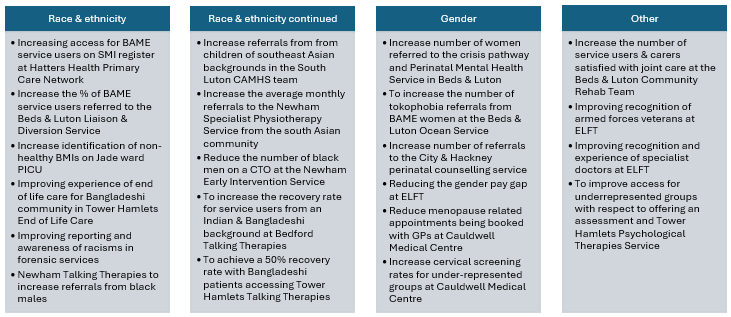
Across the programme over 22 change ideas were tested. These ideas included:
- Running cross service / organisation meetings to inform clinical cases
- Training awareness so other teams understood the purpose of a service
- Translated information and treatment materials
- A podcast to inform people about services
- Clear processes for reporting racism
- Adjusting opt in processes to make it more accessible to certain demographic groups
- Doing home visits to people who could not attend the clinic
- Sharing care plans across services
- Animated information video (click here to view)
The impact of the work was far reaching, with three teams presenting their work at international conferences. Two teams were awarded prizes for their work and four peer reviewed publications have been published or are being currently written about the work. In addition to this, several teams on the programme saw an improvement in their outcome measure, including:
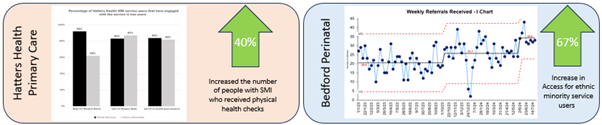
Phase three
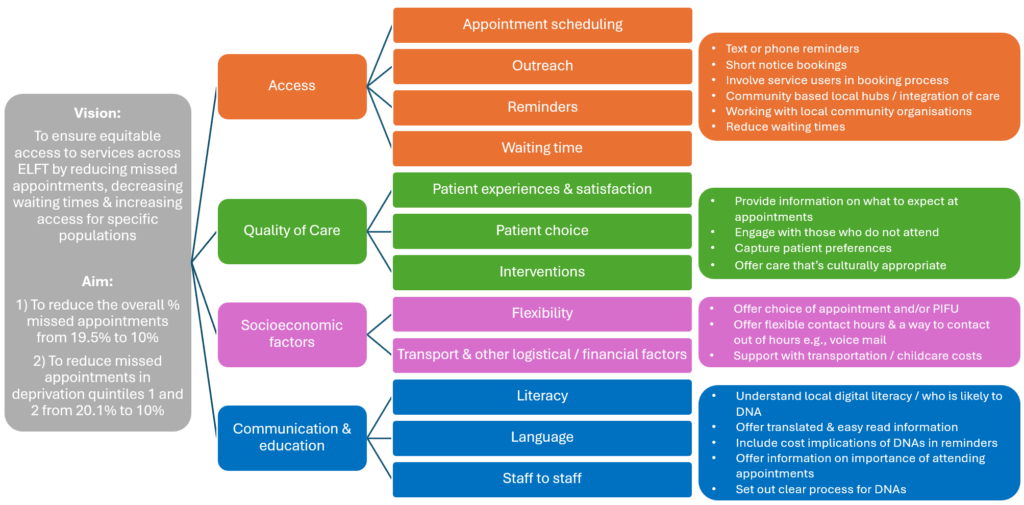
In September 2024, Phase 3 of the Pursuing Equity Programme began, bringing together 16 teams from across the Trust to tackle missed appointments. The focus was on improving access for people living in the Trust’s most deprived areas.
With the support of QI, Data & Analytics, Digital, Population Health, and People Participation, teams collaborated, innovated, and tested ideas to create more equitable healthcare and a more productive and efficient service for all.
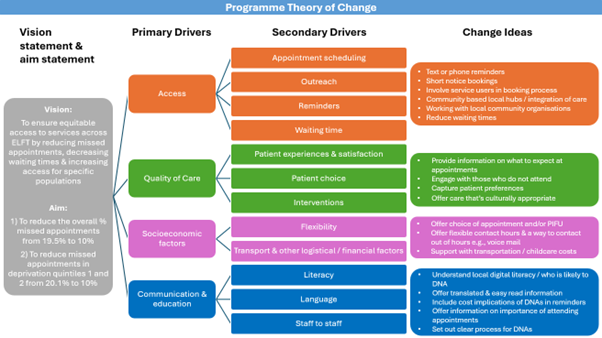
See below for the programme theory of change:
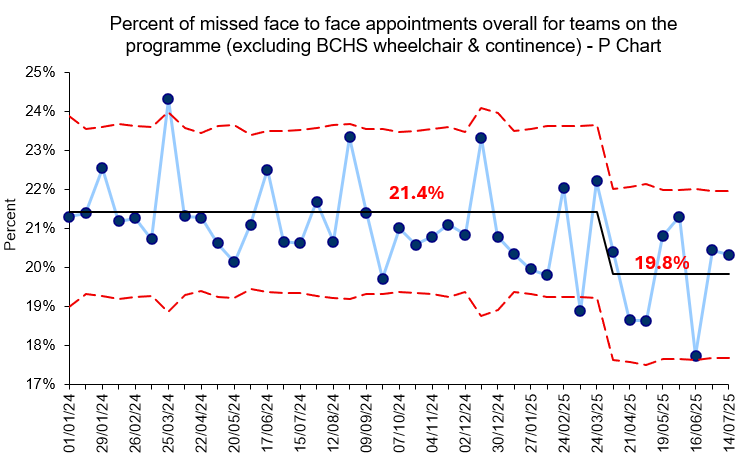
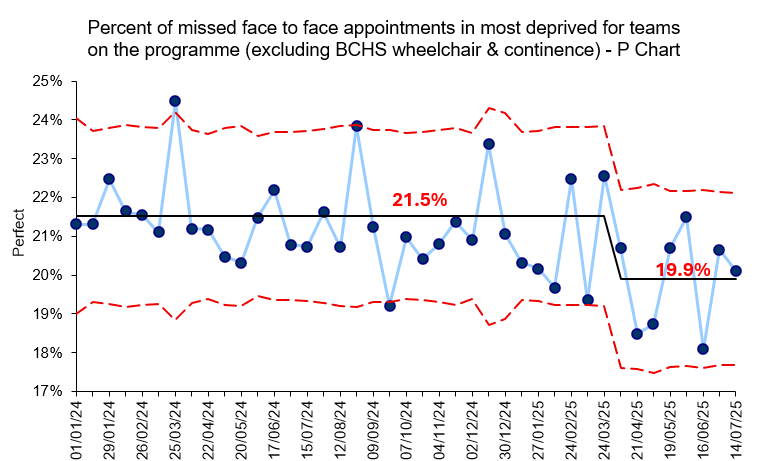
Across the programme, 13 out of the 16 teams saw an improvement in the percentage of missed face to face appointments. The proportion of missed face-to-face appointments across all teams on the programme reduced from 21.4% to 19.8%, a 7.5% overall reduction. A similar improvement was seen for those living in the most deprived areas, with missed appointments reducing from 21.5% to 19.9%.
This means that service users from the least deprived areas are now no more likely to attend than those from the most deprived areas — a key equity milestone.
Over the 11-month programme, this equated to around 43 additional appointments attended each week across the Trust.
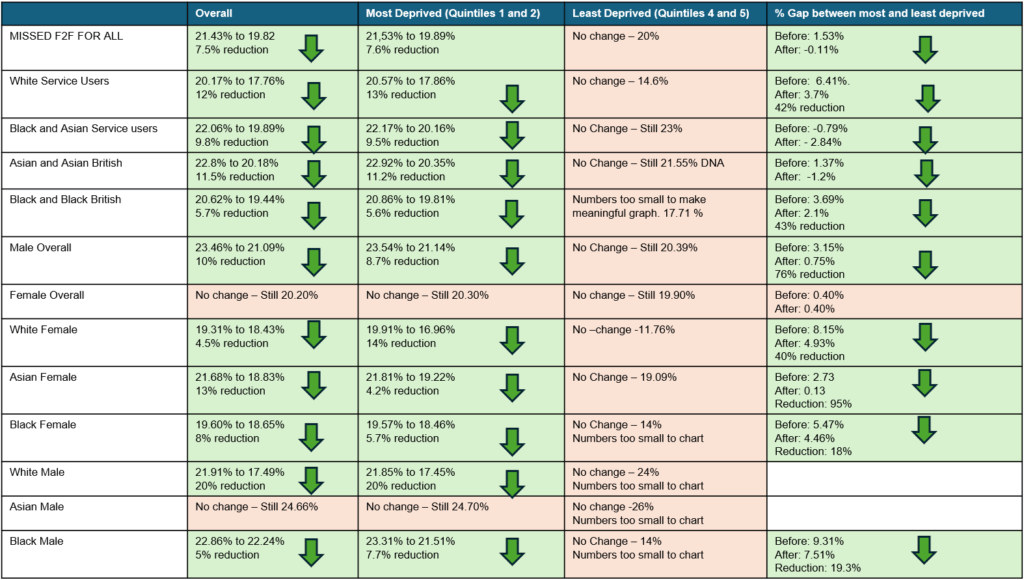
Analysis showed a consistent downward trend across most groups, with the greatest gains seen among White and Black service users.
- Overall missed appointments reduced by 7.5%, with the deprivation gap narrowing from 1.5% to below zero.
- White service users achieved a 12% reduction in missed appointments, with the equity gap between most and least deprived groups narrowing by 42%.
- Black and Asian service users saw similar improvement, with missed appointments falling by nearly 9%.
- Male service users experienced a 10% reduction, while females remained stable overall, though notable gains were observed for White and Asian women in the most deprived quintiles.
- White males from deprived communities achieved a 20% reduction in missed appointments.
See the table below for full breakdown of the results.
These results demonstrate that the reduction in missed appointments has been driven largely by improvements among service users in the most deprived quintiles, who now make up the majority of all appointments offered.
What Worked
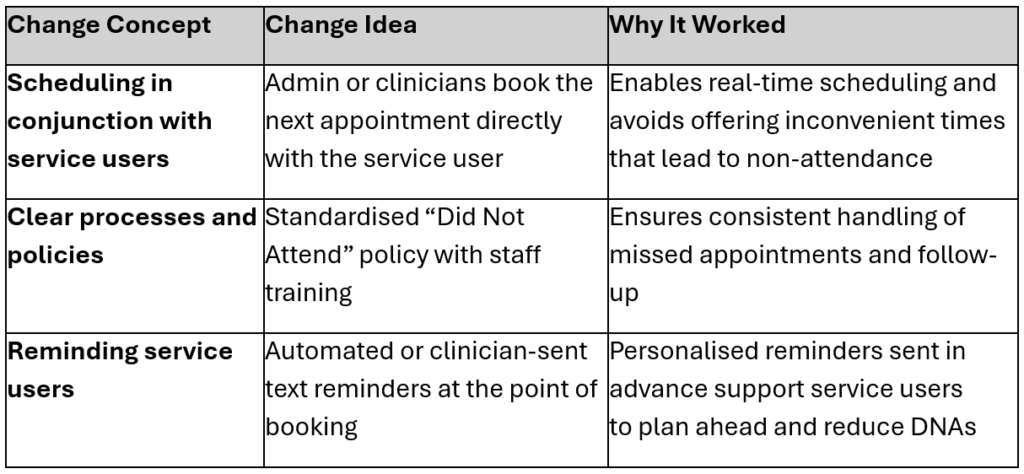
A Change Package was developed to support spread and sustainability. This included the most effective change ideas tested through the programme, which have been embedded across services:
Scaling and Sustainability
A Power BI dashboard was introduced to enable teams to monitor missed appointments in real time, ensuring that improvement is sustained. A Trust-wide Access Policy was developed setting out a consistent “ELFT Way” of managing appointments based on what has worked through this programme.
Several directorates scaled successful approaches. For example:
- CAMHS teams have embedded successful changes into local Standard Operating Procedures (SOPs).
- A joint London and Bedfordshire Community Health Services QI Forum shared learning and spread best practice.
- The Change Package was presented at the Trust Operations meeting chaired by the Chief Operating Officer and has been cascaded to all service leads.
Phase 3 of the Pursuing Equity Programme has demonstrated measurable improvement in access equity, with fewer missed appointments across the Trust and a significant narrowing of the deprivation gap. The work has generated tangible, scalable solutions, many now incorporated into standard practice, that will continue to support equitable access and optimise use of clinical time across ELFT services.
Related Stories
-
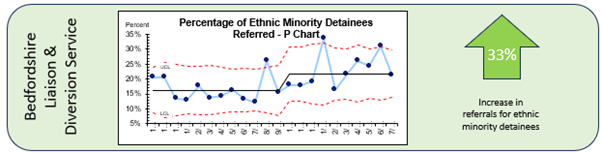
Increasing access to the Criminal Justice Liaison & Diversion Service for people from the global majority in Bedfordshire & Luton
29th January 2026

-
Enhancing Mental Health Access for Young People from South Asian Communities in Luton
22nd January 2026
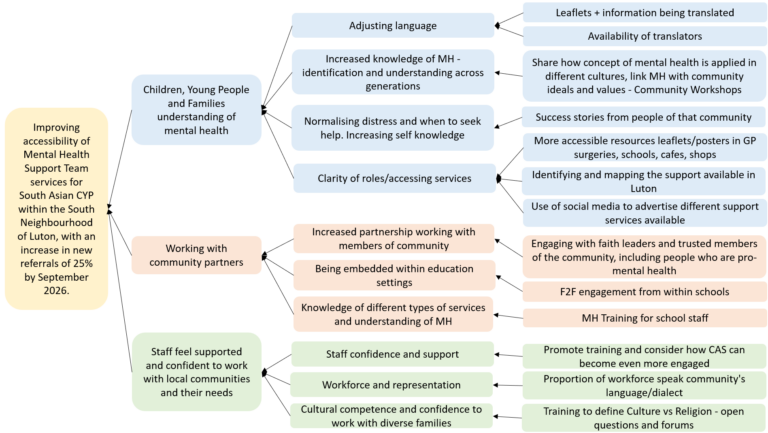
-
Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.