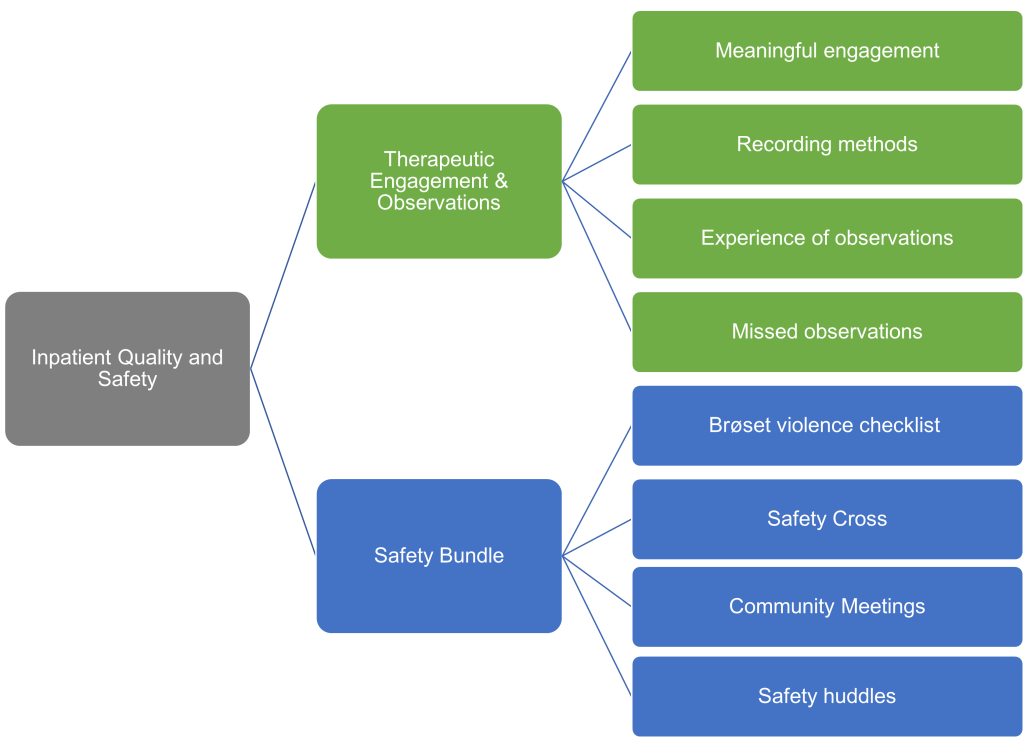
Inpatient Quality and Safety
Between 2022-2024 all inpatient wards from across the trust came together to improve quality and safety. Teams from across every part of the trust are working to make wards a more therapeutic place for service users to be. A therapeutic environment, with meaningful engagement can have positive effects for both staff and service users. An important part of this work is focusing on improving the completion of mental health observations in order to keep service users safe.
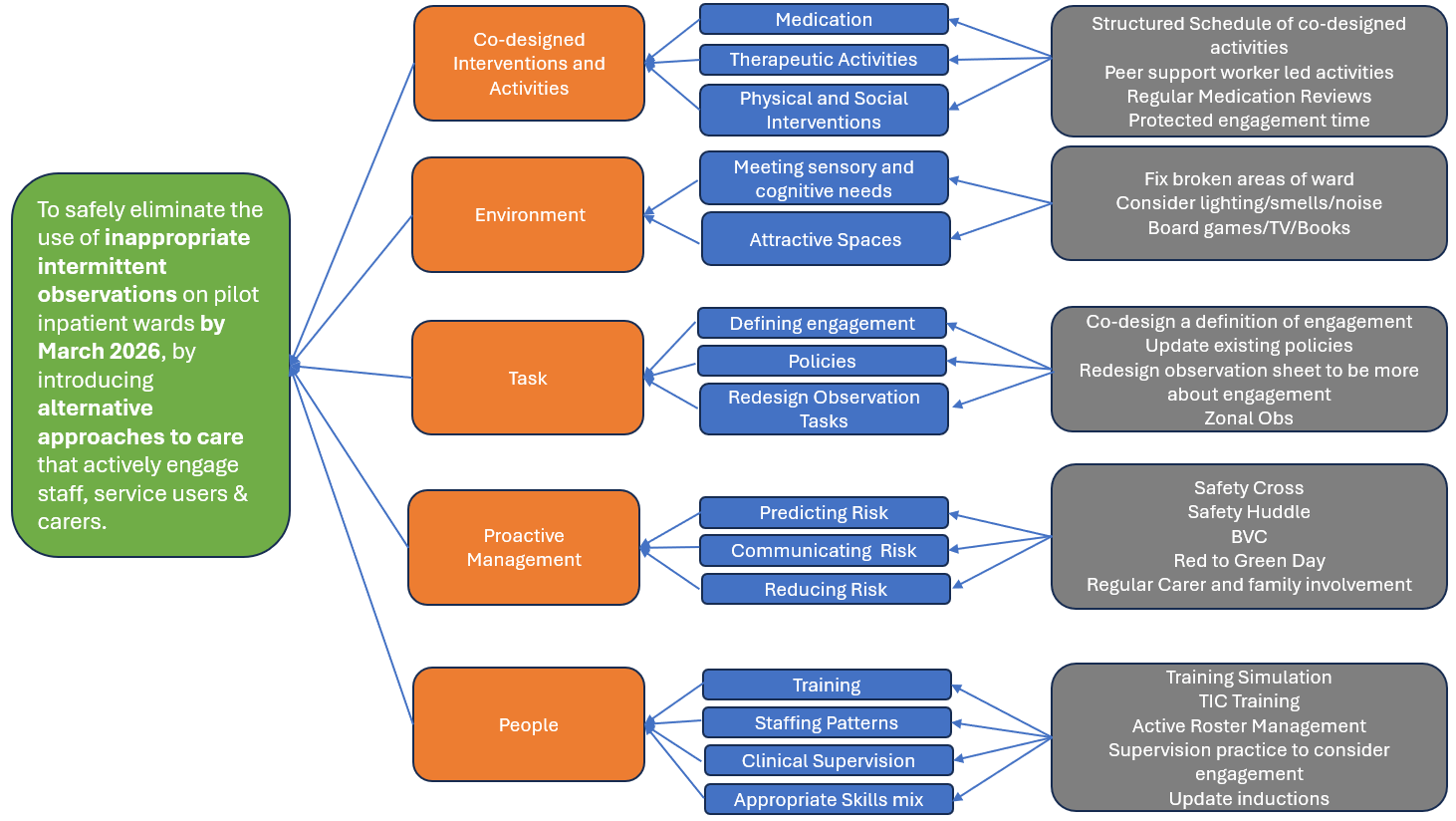
Building on previous efforts to standardise observation practices, in 2025 the Observation to Engagement Programme aimed to go further to safely eliminate the use of inappropriate intermittent observations across our inpatient mental health wards by introducing alternative approaches to care that actively engage staff, service users and carers.
Therapeutic Engagement and Observations (2022-2024)
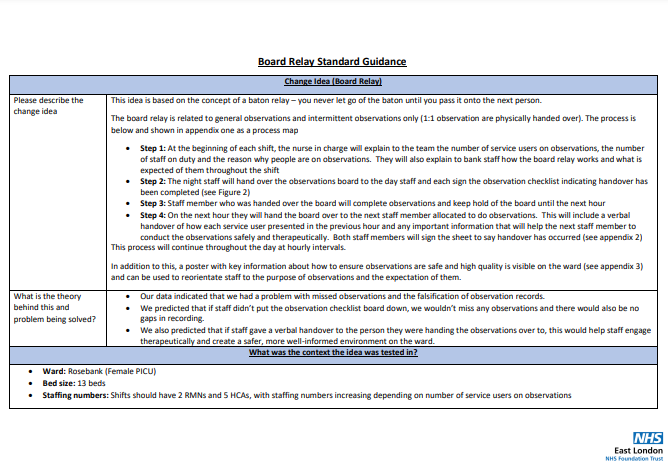
- A board relay, where staff hand over a physical board with observation documentation
- Zonal observations, where nursing staff are assigned a zone to engage with service users
- The use of Life Skills recovery workers on Twilight shifts (2 – 10pm) to conduct therapeutic activities with service users.
You can hear from staff who have been testing these ideas by watching the video below
ELFT Safety Culture Bundle
In working to strengthen the use of the safety culture bundle, teams are building on the success of work to reduce violence on inpatient wards carried out between 2014-2019 at ELFT. The bundle is made up of four parts: the safety cross, safety huddle, community meetings and the Brosset Violence checklist. You can find out more by visiting the Violence Reduction page.
From Observation to Engagement (2025 - present)
Intermittent observations have been a long-standing feature of mental health care, typically used to monitor individuals perceived to be at risk. However, growing evidence and feedback from both staff and service users suggest that this practice often brings unintended harms. These can include disrupted sleep, loss of privacy, and missed opportunities for therapeutic connection.
The figure below shows the programme-level theory of change:
The programme design
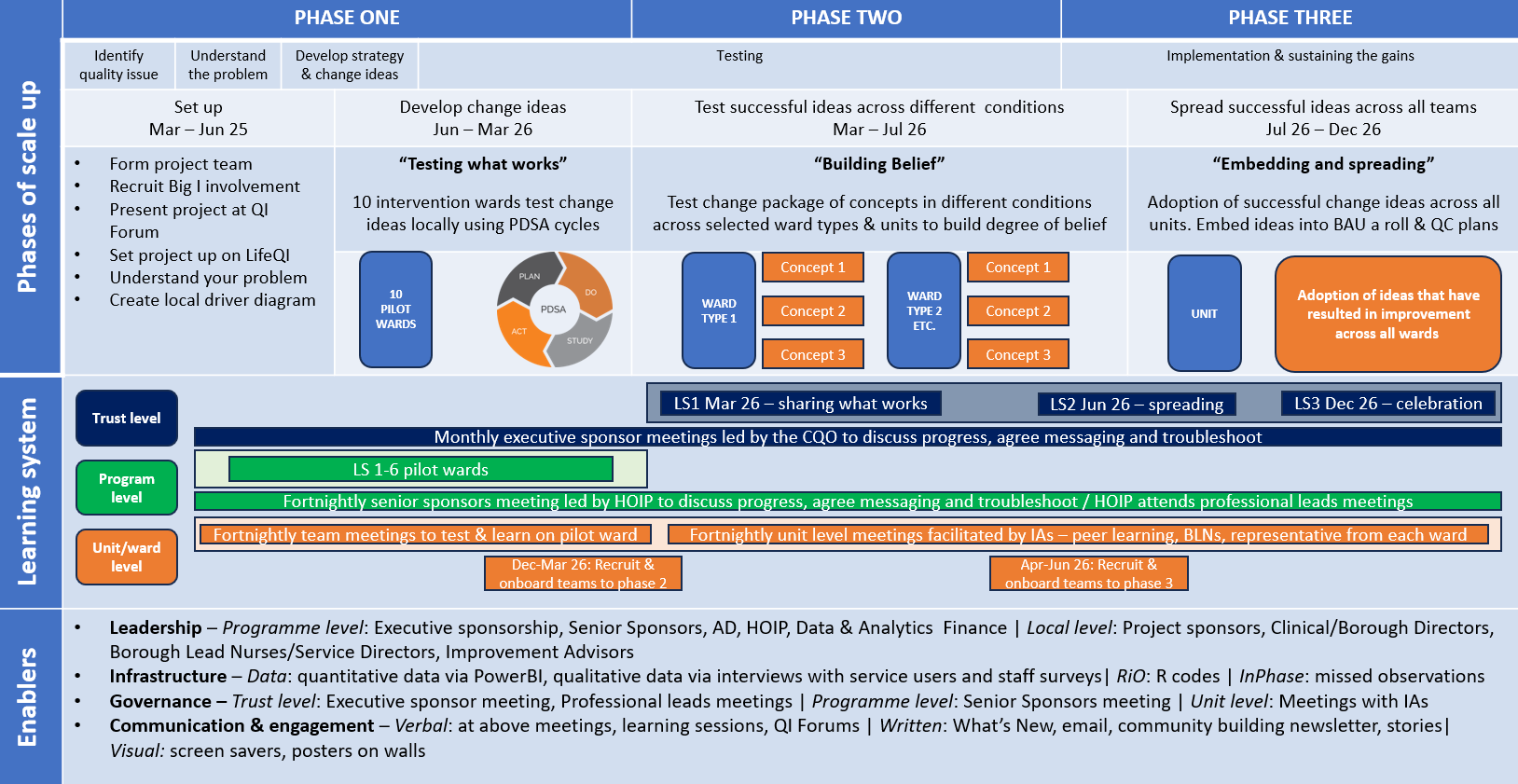
The programme will be delivered in three phases, aligned with the IHI framework for going to full scale:
- Phase 1 (April – March 2026): Ten inpatient wards tested new approaches to reducing intermittent observations with hands-on support from local Improvement Advisors, QI coaches, and sponsors. A live Power BI dashboard provided real-time data to guide decision-making and monitor impact.
- Phase 2 & 3 (March 2026 onwards): The most effective change concepts will be refined and tested in new conditions to build confidence in their effectiveness. Once a strong degree of belief is established, these concepts will be spread across all ELFT inpatient wards using a structured approach to scale up.
Test wards were paired with control wards to help understand the true impact of change. Teams met regularly to learn from each other, share successes, and overcome challenges together.
Key measures included:
- Total number of days per week service users are on enhanced observation
- Rates of safety and restrictive practice incidents (e.g. violence and aggression, seclusion, restraint, self-harm)
- Bank staffing levels
- Qualitative measures around service user and staff experience of care
The figure below shows the high-level programme design:
Related Stories
-
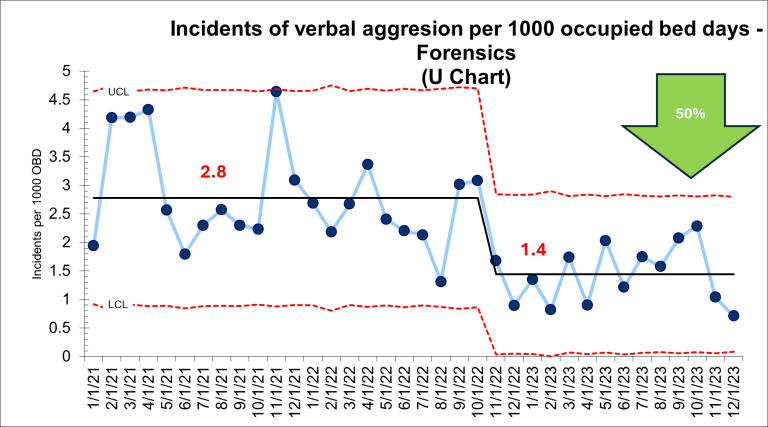
Service Users Co-Production in Observation and Therapeutic Engagement Project in Forensics Directorate
20th March 2024
-
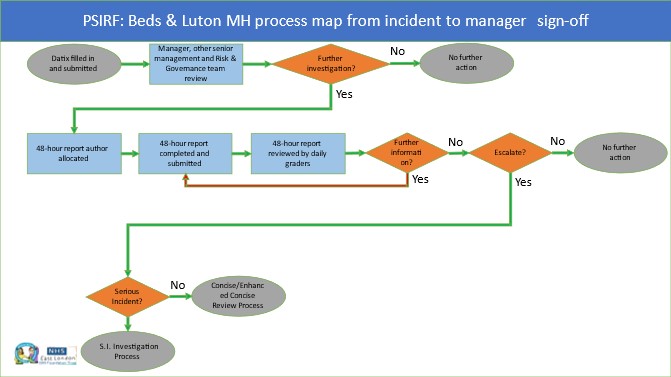
Patient safety – adopting a learning and improving approach
5th February 2024
-
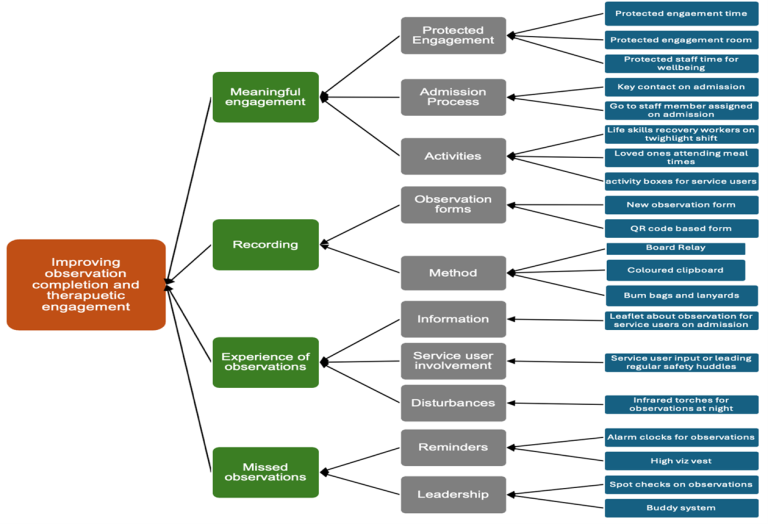
Improving observation practice and therapeutic engagement across inpatient wards at ELFT – The opportunity of using Quality Improvement at Scale
5th February 2024
Follow QI on social media
To keep up to date on the latest concerning QI at ELFT, follow us on our socials.